Psoriasis is curable.
We have tried this medicine on number of patients and achieved almost 80% results.
It is 100% safe. No chemicals. No steroids. No alkaloids. No side effects.
You need not to apply anything on skin. No ointment, no cream.
You can take it without medical prescription.
Only Herbs and Homeopathy.
Yes it is miracle.
Allopathy considers Psoriasis is incurable.
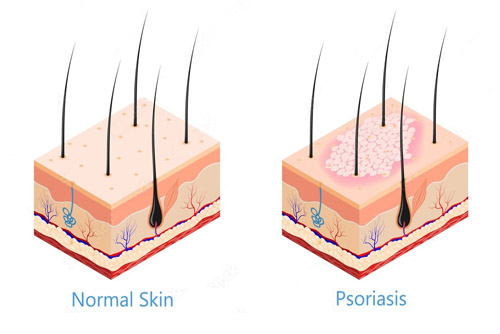
What is Psoriasis?
Psoriasis is a lifelong skin disease that occurs when faulty signals in the immune system cause skin cells to regenerate too quickly--every three to four days instead of the usual 30-day cycle. Extra skin cells build up on the skin's surface, forming red, flaky, scaly lesions that can itch, crack, bleed and be extremely painful. Psoriasis generally appears on the joints, limbs and scalp but it can appear anywhere on the body, covering some people from head to toe. More than 5 million Americans have psoriasis and/or psoriatic arthritis, a degenerative disease of the joints and connective tissues associated with psoriasis. Psoriasis typically first strikes people between the ages of 15 and 35, but can affect anyone at any age, including children.
US government is spending millions of dollars on the treatment of Psoriasis but with no effect.
Psoriasis is a long-lasting autoimmune disease characterized by patches of abnormal skin. An autoimmune disease is a condition arising from an abnormal immune response to a normal body part. These skin patches are typically red, itchy, and scaly. Psoriasis varies in severity from small, localized patches to complete body coverage.
Psoriasis is a noncontagious, chronic skin condition that produces plaques of thickened, scaling skin. Dry flakes of skin scales are the result of excessively rapid reproduction of skin cells (proliferation). The proliferation of skin cells is triggered by inflammatory chemicals produced by specialized white blood cells called T-lymphocytes.
Psoriasis has a variable course, periodically improving and worsening. It is not unusual for psoriasis to spontaneously clear for years and stay in remission. Many people note a worsening of their symptoms in the colder winter months.
Psoriasis is generally thought to be a genetic disease that is triggered by environmental factors.
Symptoms often worsen during winter and with certain medications, such as beta blockers or No steroidal anti-inflammatory drugs. These are a drug class that reduce pain, decrease fever, prevent blood clots and, in higher doses, decrease inflammation.
What causes Psoriasis?
The cause of psoriasis isn't fully understood, but it's thought to be related to an immune system problem with T cells and other white blood cells, called neutrophils, in your body.
T cells normally travel through the body to defend against foreign substances, such as viruses or bacteria.
But if you have psoriasis, the T cells attack healthy skin cells by mistake, as if to heal a wound or to fight an infection.
Overactive T cells also trigger increased production of healthy skin cells, more T cells and other white blood cells, especially neutrophils. These travel into the skin causing redness and sometimes pus in pustular lesions. Dilated blood vessels in psoriasis-affected areas create warmth and redness in the skin lesions.
The process becomes an on-going cycle in which new skin cells move to the outermost layer of skin too quickly — in days rather than weeks. Skin cells build up in thick, scaly patches on the skin's surface, continuing until treatment stops the cycle.
Just what causes T cells to malfunction in people with psoriasis isn't entirely clear. Researchers believe both genetics and environmental factors play a role.
Psoriasis triggers
Psoriasis typically starts or worsens because of a trigger that you may be able to identify and avoid. Factors that may trigger psoriasis include:
Infections, such as strep throat or skin infections
Injury to the skin, such as a cut or scrape, a bug bite, or a severe sunburn
Stress
Smoking
Heavy alcohol consumption
Vitamin D deficiency
Certain medications — including lithium, which is prescribed for bipolar disorder, high blood pressure medications such as beta blockers, antimalarial drugs, and iodides
Risk factors
Anyone can develop psoriasis, but these factors can increase your risk of developing the disease:
Family History: This is one of the most significant risk factors. Having one parent with psoriasis increases your risk of getting the disease, and having two parents with psoriasis increases your risk even more.
Viral and Bacterial Infections: People with HIV are more likely to develop psoriasis than people with healthy immune systems are. Children and young adults with recurring infections, particularly strep throat, also may be at increased risk.
Stress: Because stress can impact your immune system, high stress levels may increase your risk of psoriasis.
Obesity: Excess weight increases the risk of psoriasis. Lesions (plaques) associated with all types of psoriasis often develop in skin creases and folds.
Smoking: Smoking tobacco not only increases your risk of psoriasis but also may increase the severity of the disease. Smoking may also play a role in the initial development of the disease.
How many types of Psoriasis are?
There are five main types of psoriasis:
Plaque psoriasis
It is most common type of Psoriasis. About 80-85% of people with Psoriasis have this type.
Plaque psoriasis typically appears as raised areas of inflamed skin covered with silvery-white scaly skin. These areas are called plaques and are most commonly found on the elbows, knees, scalp, and back. It may be accompanied by severe itching, swelling, and pain. It affects all body sites, including the face, hands, feet, nails, trunk, and extremities.
Plaque psoriasis can be fatal as the extreme inflammation and exfoliation disrupt the body's ability to regulate temperature and perform barrier functions.
Pustular Psoriasis
Pustular psoriasis is an uncommon form of psoriasis. Pustular psoriasis appears as clearly defined, raised bumps that are filled with a white, thick fluid composed of white blood cells. This purulent exudate is commonly called pus. The skin under and around these bumps is red.
Types of Pustular Psoriasis
Von Zumbusch can appear abruptly on the skin. It is characterized by widespread areas of reddened skin, which become painful and tender. Within hours, the pustules appear. In next 24 to 48 hours the pustules dry, leaving the skin with a glazed and smooth appearance. Von Zumbusch is associated with fever, chills, severe itching, dehydration, a rapid pulse rate, exhaustion, anemia, weight loss and muscle weakness.
Palmoplantar pustulosis (PPP) causes pustules on the palms of the hand and soles of the feet. It commonly affects the base of the thumb and the sides of the heels. Pustules initially appear in a studded pattern on top of red plaques of skin, but then turn brown, peel and become crusted. PPP is usually cyclical, with new crops of pustules followed by periods of low activity.
Acropustulosis (acrodermatitis continua of Hallopeau) is a rare type of psoriasis characterized by skin lesions on the ends of the fingers and sometimes on the toes. The eruption occasionally starts after an injury to the skin or infection. The lesions can be painful and disabling, and cause deformity of the nails. Occasionally bone changes occur in severe cases.
Inverse psoriasis
Inverse psoriasis (also known as flexural psoriasis) appears as smooth, inflamed patches of skin. The patches frequently affect skin folds, particularly around the genitals (between the thigh and groin), the armpits, in the skin folds of an overweight abdomen known as panniculus, between the buttocks in the intergluteal cleft, and under the breasts in the inframammary fold. Heat, trauma, and infection are thought to play a role in the development of this atypical form of psoriasis.
Inverse psoriasis is found in the armpits, groin, under the breasts and in other skin folds on the body.It is particularly subject to irritation from rubbing and sweating because of its location in skin folds and tender areas. It usually lacks the scale associated with plaque psoriasis due to the moist environment. It is more common in overweight people and people with deep skin folds.
Guttate psoriasis
Guttate psoriasis (also known as eruptive psoriasis) is a type of psoriasis that presents as small (0.5–1.5 cm in diameter) lesions over the upper trunk and proximal extremities; it is found frequently in young adults. The term "guttate" is used to describe the drop-like appearance of skin lesions. Guttate psoriasis is classically triggered by a bacterial infection, usually an upper respiratory tract infection.
This form of psoriasis appears as small, red, separate spots on the skin. Guttate lesions usually appear on the trunk and limbs and can number in the hundreds. Sometimes lesions form on the scalp, face and ears. They usually are not as thick as the lesions that characterize plaque psoriasis. This form can precede or co-exist with other forms of psoriasis, such as plaque.
Psoriatic arthritis
Psoriatic arthritis is a form of chronic inflammatory arthritis that has a highly variable clinical presentation and frequently occurs in association with skin and nail psoriasis. It typically involves painful inflammation of the joints and surrounding connective tissue and can occur in any joint, but most commonly affects the joints of the fingers and toes. This can result in a sausage-shaped swelling of the fingers and toes known as ductility’s. Psoriatic arthritis can also affect the hips, knees, spine (spondylitis), and sacroiliac joint (sacroiliitis). About 30% of individuals with psoriasis will develop psoriatic arthritis. Skin manifestations of psoriasis tend to occur before arthritic manifestations in about 75% of cases.
Nail Psoriasis
Psoriasis can affect fingernails and toenails, causing pitting, abnormal nail growth and discoloration. Psoriatic nails might loosen and separate from the nail bed (onycholysis). Severe cases may cause the nail to crumble.
Nail psoriasis occurs in 40–45% of people with psoriasis affecting the skin and has a lifetime incidence of 80–90% in those with psoriatic arthritis. These changes include pitting of the nails (pinhead-sized depressions in the nail is seen in 70% with nail psoriasis), whitening of the nail, small areas of bleeding from capillaries under the nail, yellow-reddish discoloration of the nails known as the oil drop or salmon spot, thickening of the skin under the nail (subungual hyperkeratosis), loosening and separation of the nail (onycholysis), and crumbling of the nail.
Where does psoriasis show up?
Psoriasis can show up anywhere—on the eyelids, ears, mouth and lips, skin folds, hands and feet, and nails. The skin at each of these sites is different and requires different treatments.
Light therapy or topical treatments are often used when psoriasis is limited to a specific part of the body. However, doctors may prescribe oral or injectable drugs if the psoriasis is widespread or greatly affects your quality of life. Effective treatments are available, no matter where your psoriasis is located.
Description: Common areas of the body where psoriasis symptoms occur
Scalp Psoriasis can be very mild, with slight, fine scaling. It can also be very severe with thick, crusted plaques covering the entire scalp. Psoriasis can extend beyond the hairline onto the forehead, the back of the neck and around the ears.
Face Facial psoriasis most often affects the eyebrows, the skin between the nose and upper lip, the upper forehead and the hairline. Psoriasis on and around the face should be treated carefully because the skin here is sensitive.
Hands, Feet and Nails Treat sudden flares of psoriasis on the hands and feet promptly and carefully. In some cases, cracking, blisters and swelling accompany flares. Nail changes occur in up to 50 percent of people with psoriasis and at least 80 percent of people with psoriatic arthritis.
Genital Psoriasis
The most common type of psoriasis in the genital region is inverse psoriasis, but other forms of psoriasis can appear on the genitals, especially in men. Genital psoriasis requires careful treatment and care.
Skin Folds
Inverse psoriasis can occur in skin folds such as the armpits and under the breasts. This form of psoriasis is frequently irritated by rubbing and sweating.
How severe is my psoriasis?
Psoriasis can be mild, moderate or severe. Your treatment options may depend on how severe your psoriasis is. Severity is based on how much of your body is affected by psoriasis. The entire hand (the palm, fingers and thumb) is equal to about 1 percent of your body surface area.
However, the severity of psoriasis is also measured by how psoriasis affects a person's quality of life. For example, psoriasis can have a serious impact on one's daily activities even if it involves a small area, such as the palms of the hands or soles of the feet.